Introduction :-
Tall Stature :-
Short Stature :-
2.Body Proportions :-
3.Nutrition :-
4.Decubitus :-
5.Skin,Hair & Nails :-
Examination of Hair :
Examination of Nails :
6.Clubbing :-
7.Cyanosis :-
8.Jaundice :-
9.Pallor :-
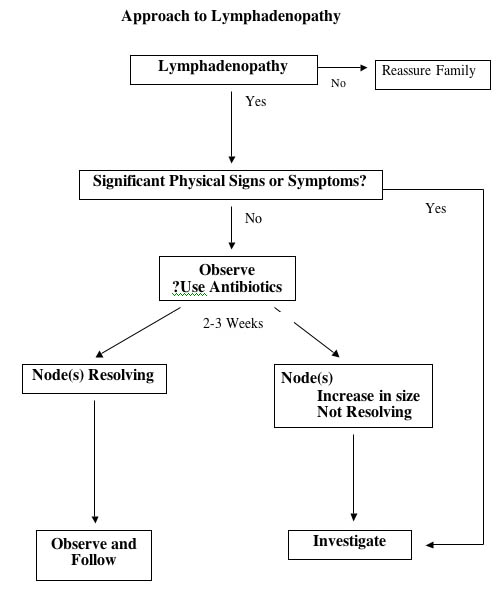
10.Lymphadenopathy :-


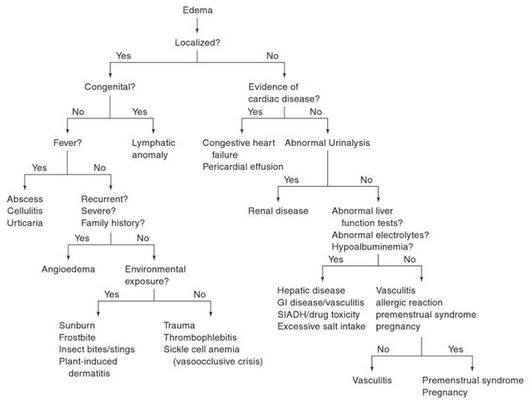
11.Edema :-

12.Vertebral column :-


13.Thickened nerves :-
15.Temperature :-




16.Pulse :-



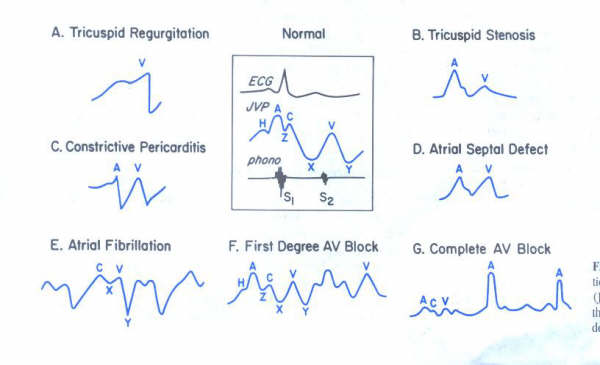


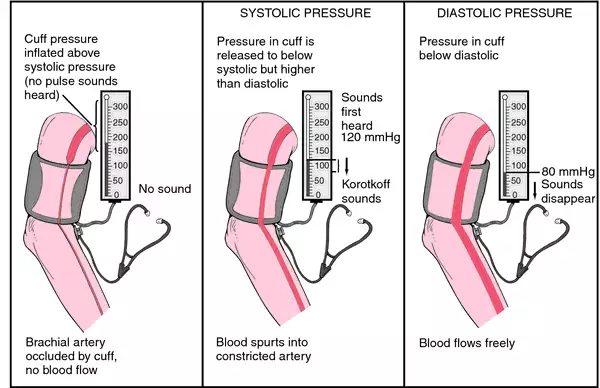
17.Blood Pressure :-


- The general examination of the patient must be done systematically, noting the following -
- Built
- Nutrition
- Skin, hair and nails
- Lymphadenopathy
- Edema
1.Built :-
- Built is the skeletal structure in relation to age and sex of the individual as compared to a normal person.

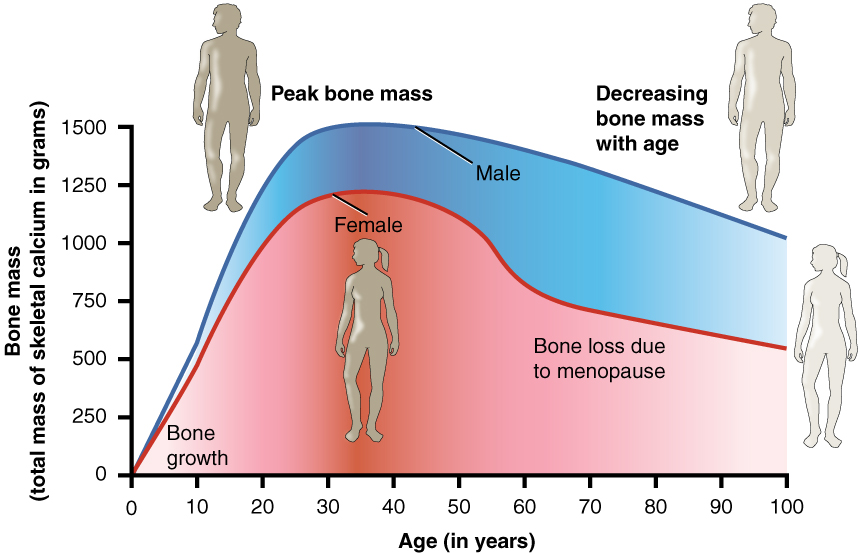
Tall Stature :-
- A child is considered to be tall when the height is greater than 2 standard deviations above the mean for the age. Gigantism is the term applied when the patient's height is greatly in excess of the normal for his age before fusion of epiphysis. There is no fixed height to continue a giant, but in adults, it is applied for individuals with a height of more than 61/2 Ft.
Short Stature :-
- Dwarfism is the term applied when the patient's height is 2 standard deviations less than that for his/her age and sex. mid-parental height usually determines the final height.
2.Body Proportions :-
- Normally, in adults, the height of the person is equal to the length of arm span. The upper segment ( from vertex to the pubic symphisis ) is equal to the lower segment ( from pubic symphisis to the heel ).
- In infants, the upper segment is greater than the lower segment and the height is greater than the arm span. This infantile type of body proportion persists in achondroplasia, cretinism and juvenile myxedema.
- The reverse of infantile body proportion i.e. arm span greater than height and lower segment greater than upper segment occurs in eunuchoidism, marfan's syndrome, homocystinuria, klinefelter's syndrome and frohlich's syndrome.
3.Nutrition :-
- A normal person is well nourished as regards proteins, fats, carbohydrates, vitamins and minerals. certain clinical signs help to diagnose deficiency of one or more of these nutrients.
- Proteins :- Hypoproteinemia causes rough skin and later edema of feet and brittle hair.
- Fats :- Fat malnutrition leads to cachexia with hollowing of cheeks, loss of the shape of hips ( due to loss of fats ), flat abdomen and absent fat over the subcutaneous tissues of the elbows.
- Carbohydrates :- Carbohydrate malnutrition is difficult to detect clinically because there is gluconeogenesis from fats or proteins.
- Vitamins :- These can be fat soluble ( vitamin A, D, E, K ) or water soluble (rest).
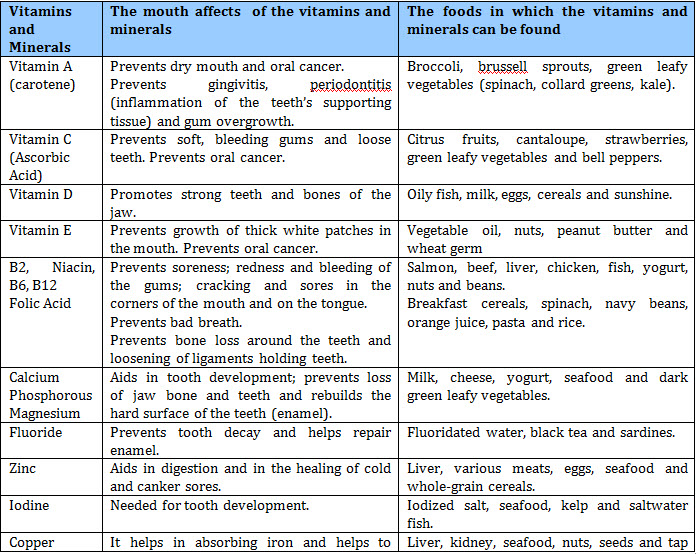
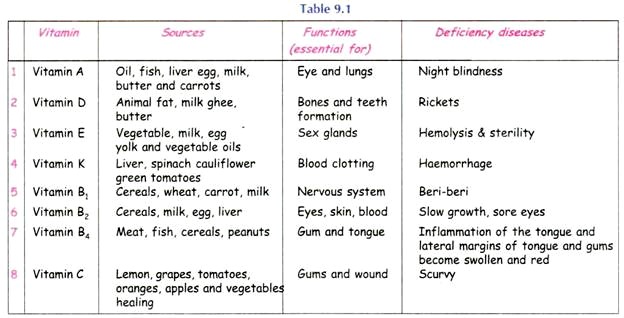

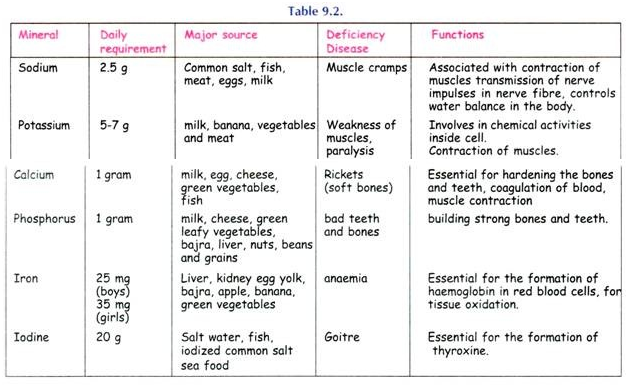
- Minerals :- Deficiency of two minerals can be diagnosed clinically. Iron deficiency causes koilonychia and pallor whereas calcium deficiency causes tetany.
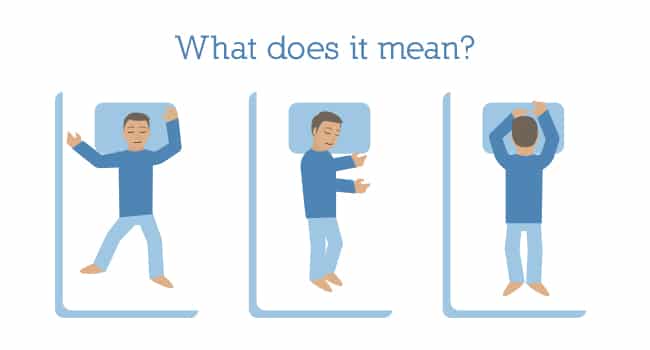
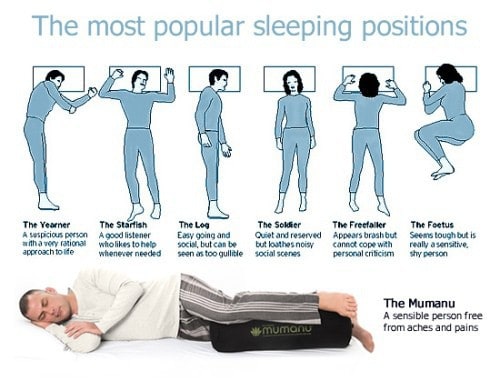
4.Decubitus :-
- Decubitus or the posture a patient adopts when lying in bed often gives a valuable diagnostic clue.
- Hemiplegia :- The patient lies in bed with one side immobile, the affected arm flexed and the affected leg externally rotated and extended.
- Meningitis and tetanus :- The patient has neck stiffness and opisthotonos.
- Colic :- In renal, biliary or intestinal colic, the patient is markedly restless and tossing and turning in bed in agony.
- Acute inflammatory abdominal disease :- The patient lies on his back quietly with legs drawn up.
- Cardiorespiratory embarrasment :- The patient is more comfortable in sitting-up position. This position is also assumed in abdominal distention and ascites when intra-abdominal pressure is raised.
- Pneumonia and pleurisy :- The patient is most comfortable lying on the affected side because the movement on the affected side is restricted.
5.Skin,Hair & Nails :-
Examination of skin often gives important clues to local or systemic diseases. The following features should be noted :
- Color :- It may be pale, flushed, cyanosed, yellow etc.
- Pigmentation :- Pigmentation may occur in several diseases. some common medical conditions associated with pigmentation are :
- Endocrine : Addison's disease, cushing's disease, thyrotoxicosis.
- Deficiency : pellagra, kwashiorkor, megaloblastic anemia.
- Infections : kala azar, chronic malaria, secondary syphilis, tuberculosis, leprosy, HIV etc.
- Metabolic : Hemochromatosis.
- Skin disease : neurofibromatosis, lichen planus, acanthosis nigricans etc.
- Miscellaneous : Malignancy, pernicious anemia, exposure to sunrays or radiations.
- Hypopigmentation :- Hypopigmented patches may occur in leprosy, leukoderma, albinism, fungal infections of skin, etc.
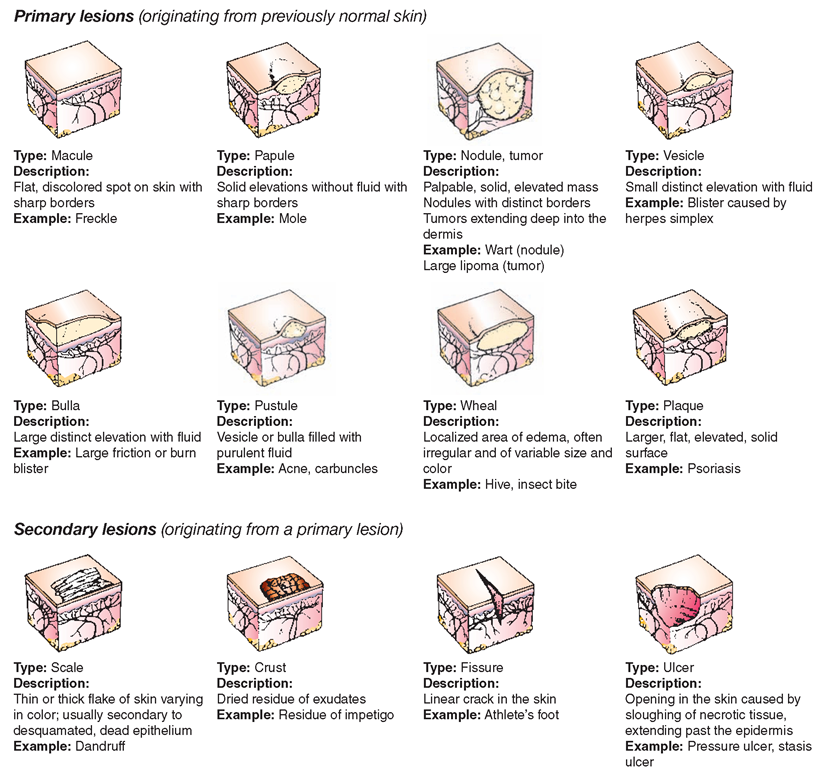
- Eruptions : various types of eruptions may occur as follows:
Examination of Hair :
 |
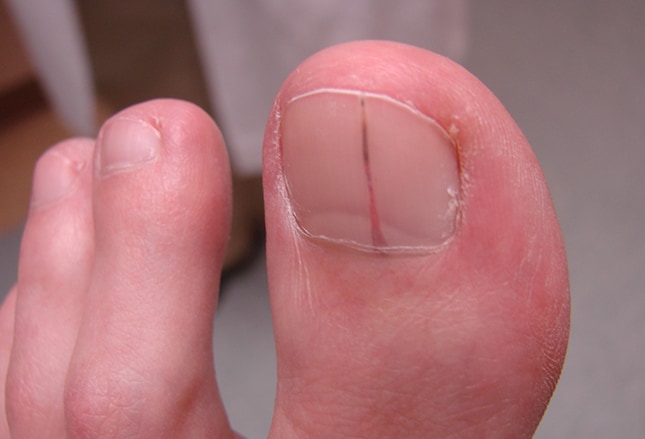
Examination of Nails :
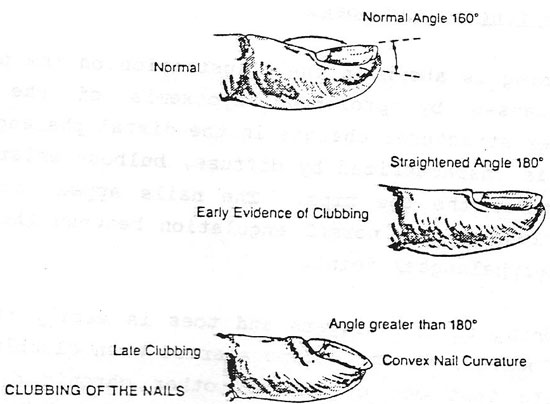
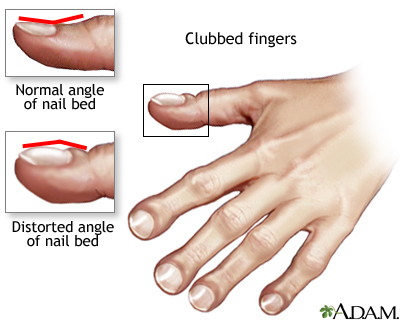
6.Clubbing :-
7.Cyanosis :-
8.Jaundice :-
9.Pallor :-
- pallor is paleness of skin and mucous membrane either as a result of diminished circulating red blood cells or diminished blood supply.
Paleness should be distinguished from other causes of prominent white skin:
- Fair skin is genetically determined skin hue with low concentration of skin pigment (melanin) in the skin. This skin hue is common in people in north European countries (Germany, Great Britain, Ireland, Scandinavian countries).
- Absence of skin tan from sun avoidance.
- Myxedema (in hypothyroidism) – swelling of under-skin tissues causes pale appearance of the skin.
- Albinism is a rare genetic disorder with partial or complete lack of melanin in the skin, hair and iris of the eye. Affected persons have white skin and hair, and red iris.
- Vitiligo is a patchy loss of skin color due to destruction of pigment cells (melanocytes) from an unknown cause.
Everyday Causes of Paleness
Paleness does not always mean you are ill.
- When exposed to low environmental temperature, your face, palms or other body parts may become pale because of narrowing (constriction) of the small skin arteries as part of a body’s heat-saving process.
- When you keep your arms or legs above the level of the heart for a minute, they may become pale (and numb or tingling), since the power of the heart can not efficiently pump the blood into the limbs against the force of gravitation.
- Skipped meal and resulting drop of glucose blood level, or dehydration, may trigger adrenalin release and constriction of your skin arteries.
- In exertion or fear, blood is redirected from the skin to muscle arteries. Your skin may remain pale for several minutes after exertion.
Sudden Paleness
Health disorders, causing sudden paleness (within minutes to hours) all over the body:
- Orthostatic hypotension – temporary fall of blood pressure after standing up after prolonged sitting or lying.
- Stomach upset from wrong food combination, alcohol or food poisoning
- Dehydration from insufficient drinking, excessive sweating, vomiting, diarrhea
- Acute infection (usually with fever)
- Fainting (vasovagal syncope) due to strong pain, emotions, heat or unpleasant sensations
- Motion sickness
- Allergy to drugs
- Rapid stomach emptying (dumping syndrome)
- Migraine
- Heat stroke
- Hypothermia
- Heart failure due to heart attack, arrhythmia, infective endocarditis or other heart disorder, when the heart can not efficiently pump the blood into the circulation
- Low blood sugar (hypoglycemia), common in insulin-dependent diabetics after an exercise, skipped meal or insulin overdose
- Blood loss due to external or internal bleeding (in car accidents, shooting or stitch injuries), heavy menstrual bleeding, surgery
- Hypothermia
- Shock - a sudden, deep fall of blood pressure - due to poisoning, severe infection, burns, severe blood loss
- Side effect of medications:
- warfarin, corticosteroids, aspirin and other anti-rheumatic drugs may cause intestinal bleeding
- iron poisoning
- Drug overdose: amphetamine (speed), cocaine
- Chemical poisoning (pesticides), plant poisoning (Atropa belladonna)
- Death
Sudden Paleness in Limbs
Health disorders, causing sudden paleness in limbs:
- Raynaud’s disease and Raynaud’s phenomenon caused by exposure to cold, ergotamin, etc.
- Chilblains or frostbite
- Acute arterial occlusion
- Limb swelling after injury or surgery (compartment syndrome)
Long Lasting Paleness
Paleness lasting from few weeks to several years and affecting the whole body may result from:
- Low blood pressure, insufficient to keep small skin arteries open
- Anemia due to iron or vitamin B12 and folate deficiency due to
- low intake: vegetarians, irregular diet, starvation, alcoholism
- impaired absorption: Crohn’s or celiac disease
- intestinal parasites
- intestinal bleeding: colorectal cancer, ulcerative colitis
- heavy menstrual bleeding
- hemolysis
- drugs phenytoin and methotrexate
- chronic kidney disease
- chemotherapy
- cancer in advanced stage
- chronic hepatitis or liver cirrhosis
- pregnancy
- Hypertension
- Chronic heart failure after heart attack, heart valve disorders, etc.
- Side effect of medications:
- warfarin, aspirin, ibuprofen, naproxen, corticosteroids may cause intestinal bleeding
- iron poisoning
- Drug abuse: amphetamine (speed), cocaine
- Thrombosis and other blood clotting disorders
- Leukemia, lymphoma, Hodgkin disease
- Hypopituitarism - impaired production of pituitary hormones, mainly due to pituitary adenoma
Long Lasting Paleness in Limbs
- Chronic arterial occlusion
- Carpal tunnel syndrome
- Acromegaly
Paleness in Children
Disorders, commonly or mainly causing paleness in children:
- Dehydration
- Stress from travel
- Childhood diseases with fever
- Iron deficiency anemia
- Malnutrition due to starvation or lack of proteins in the diet
- Rheumatic fever
- Congenital heart disorders
- Cystic fibrosis
- Genetic metabolic disorders: phenylketonuria
- Lymphadenopathy is inflammatory or non-inflammatory enlargement of lymphnodes.



11.Edema :-


12.Vertebral column :-


13.Thickened nerves :-
- It may be due to
- leprosy
- Diabetes
- Amylodosis
- Charcot marie tooth syndrome
- Sarcoidosis
- Refsum's Disease
- Rusy Levy Syndrome
- Dejerine sotta's syndrome
- Idiopathic hypertrophic neuropathy
14.Joints :-
- CIDP ( Chronic Inflammatory Demylinating polyneuropathy )
15.Temperature :-




16.Pulse :-




17.Blood Pressure :-



Take Care Of Your Body,
It's The Only Place You Have To Live In.
With Best Regards, Karnav Thakkar :) :)


















.jpg)





No comments:
Post a Comment