Introduction :-













The abdominal exam, in medicine, is performed as part of a physical examination, or when a patient presents with abdominal pain or a history that suggests an abdominal pathology.
The abdominal exam has conventionally been split into different stages:
- Positioning of the patient and their environment.
- Inspection of the patient and their anterior and posterior abdomen.
- Auscultation of the abdomen with a stethoscope.
- Palpation of the patient's abdomen and its organs.
- Percussion of the patient's abdomen.
- Special tests inspecting for signs of various liver diseases.

When accompanying other physicians or students, medical staff typically report as they examine a patient. An example normal examination may include:
- adjustment of environment
- "on inspection, the abdomen is non-distended and there are no signs of liver disease"
- "bowel sounds are present"
- "the abdomen is soft and non-tender, with no organomegaly"
- "no rebound tenderness"

Positioning and Environment :-
- Position is patient should be supine and the bed or examination table should be flat. The patient's hands should remain at his/her sides with his/her head resting on a pillow. If the neck is flexed, the abdominal musculature becomes tensed and the examination made more difficult. Allowing the patient to bend his/her knees so that the soles of their feet rest on the table will also relax the abdomen.
- Lighting is adjusted so that it is ideal.
- Draping is patient should be exposed from the pubic symphysis below to the costal margin above - in women to just below the breasts. Some surgeons would describe an abdominal examination being from nipples to knees.
- Although physicians have had concern that giving patients pain medications during acute abdominal pain may hinder diagnosis and treatment.

Inspection:-

The abdominal exam typically begins with the examiner inspecting the patient, paying particular attention to any signs of liver disease. These signs (stigmata) may include
- General: spider angiomata, temporal wasting, fetor hepaticus, asterixis (flapping tremor)
- Hands: clubbing, thenar wasting, Dupuytren's contracture, palmar erythema
- Estrogen related: spider nevi
- Estrogen-related in males: testicular atrophy, gynecomastia
- Associated with portal hypertension: hematochezia (blood in stool), hematemesis - gastric bleed, esophageal varices,caput medusae (rare) - venous distension, ascites
The patient is also examined for:
- masses
- scars, sinuses
- lesions
- signs of trauma
- bulging flanks
- jaundice/scleral icterus
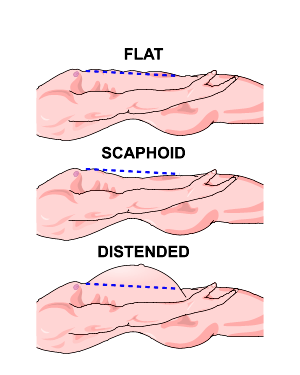
- abdominal distension
- caput medusae
- cough impulse
Auscultation:-

- Auscultation refers to the use of a stethoscope by the examiner to listen to the abdomen.
- Auscultation is performed prior to palpation of the abdomen as it is least likely to elicit pain.
- The doctor warms the diaphragm of the stethoscope, and listens to the bowel sounds. Some controversy exists as to the length of time required to confirm or exclude bowel sounds, with suggested durations up to five minutes. Bowel obstruction may present with grumbling bowel sounds or high-pitched noises. Absence of sounds may be caused by peritonitis.
- The examiner also typically listens to the two renal arteries for bruits by listening in each upper quadrant, adjacent to and above the umbilicus. Bruits heard in the epigastrium that are confined to systole are considered normal.

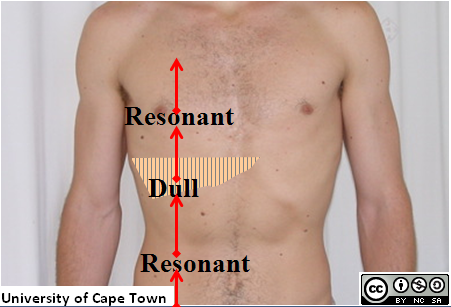
Percussion:-



Percussion is performed by knocking the middle finger against the phalanx of the middle finger of the opposing hand, which rests against the surface of the abdomen in each of the nine areas tested. Percussion can elicit a painful response in the patient, and may also reveal whether there is abnormal levels of fluid in the abdomen. Organomegaly may also be noted, including gross splenomegaly (enlargement of the spleen), hepatomegaly (enlargement of the liver), and urinary retention.
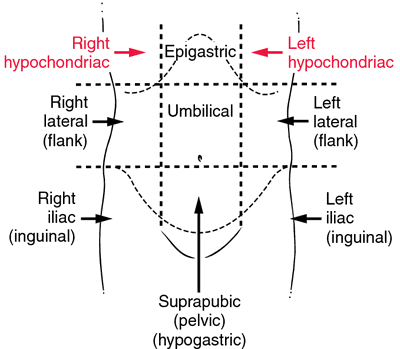
The examiner, when percussing for organomegaly, percusses in a particular manner:
- percuss the liver from the right iliac region to right hypochondrium
- percuss for the spleen from the right iliac region to the right hypochondrium and the left iliac to the left hypochondrium.
Examination of the spleen
- Castell's sign or alternatively Traube's space
Palpation:-


The examiner typically palpates all nine areas of the patient's abdomen. This is typically performed twice, lightly and then deeply.
On light palpation, the examiner tests for any palpable mass, rigidity, or pain.
On deep palpation, the examiner is testing for and organomegaly, including enlargement of the liver and spleen.

Reactions that may indicate pathology include:
- guarding, describing muscle contraction as pressure is applied.
- rigidity, indicating peritoneal inflammation.
- rebound, pain on release
- hernial orifices if positive cough impulses.
Other & Special Maneuvers:-



- Examination of pelvic lymph nodes
- Digital rectal exam - Abdominal examination is not complete without a digital rectal exam.
- Pelvic examination only if clinically indicated.
Special manevures may also be performed, to elicit signs of specific diseases. These include
- Appendicitis or peritonitis:
- Psoas sign - pain when tensing the psoas muscle
- Obturator sign - pain when tensing the obturator muscle
- Rovsing's sign - pain in the right iliac fossa on palpation of the left side of the abdomen
- Carnett's sign - pain when tensing the abdominal wall muscles
- Patafio's sign - pain when the patient is asked to cough whilst tensing the psoas muscle
- Cough test - pain when the patient is asked to cough
- Suspected Pyelonephritis: Murphy's punch sign
- Hepatomegaly: Liver scratch test
- Ascites: bulging flanks, fluid wave test, shifting dullness



Take Care Of Your Body,
It's The Only Place You Have To Live In.
With Best Regards, Karnav Thakkar :) :)

Thanks for this. I'm hving a surgery short case. 👍
ReplyDelete